
Our Complex Immune Systems
- By Sharon Erdrich
- Immune Function, Topics

Your immune system is complex. It is regulated by your genetic makeup and is heavily influenced by an interplay between diet, stress, lifestyle and environment. While there are numerous nutrients and factors involved in the healthy functioning of your immune systems, there is no single elixir to optimise it, just the symbiotic relationship of all these factors acting together. Look at each of them.
Vitamin D
For a long time, it was believed that vitamin D was only needed for absorption of calcium and therefore a requirement for normal bone development. However, not only have we learned that vitamin D is not actually a vitamin at all (it’s a steroid hormone) but we also understand that it is important for far more than just the growth and development of the skeleton.
Vitamin D has been found to adapt the immune response. Without enough of it, autoimmune conditions can be triggered, and you can be more susceptible to infections. In fact, evidence shows that a person is at higher risk of respiratory infections when they are vitamin D deficient and supplementation can protect against acute respiratory tract infection
Small amounts of vitamin D can be obtained from a few foods. It’s a fat-soluble substance, so you’ll get a little from oily fish (kahawai, sardines, tuna, salmon), egg (the yolk), meats and offal (especially liver & kidney).
Produced in the skin when exposed to sunlight, vitamin D levels peak during summer if exposure has been adequate. How much sunshine you need will vary according to your natural skin tone. As a general guide, safe sun exposure includes a little time in the sun, with arms & legs uncovered, for 5-10 minutes. This should not be long enough for you to even go pink.
Levels tend to fall during winter, the time when susceptibility to infection increases. So, in early autumn, vitamin D levels of most will be at their maximum. It is hard to build levels during winter, but you can try to keep vitamin D stores from falling too quickly by getting outside as much as possible, with some skin seeing the sun!

Zinc
This mineral is a very important micronutrient (meaning you don’t need much), and a deficiency of it can result in an impaired immune response.
There is evidence to suggest that by taking a zinc supplement within 24 hours of a cold commencing, it can reduce the severity and duration of the illness.
Zinc needs are higher in teenagers and in males. It is found in seafood (especially oysters), meat, beans/pulses and in pumpkin kernels.
Vitamin C
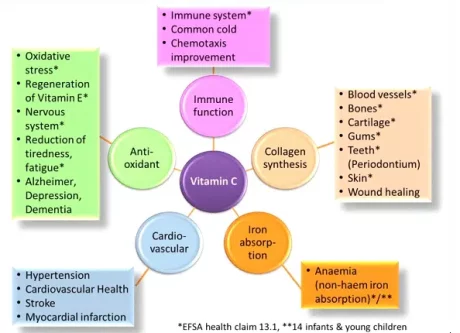
Vitamin C has a critical role in the normal function of the immune system. Not only is it required for normal function of neutrophils (a type of white blood cell that is a “first responder” in acute infection), it also aids healing by its role in making collagen. Vitamin C is also an antioxidant. Antioxidants scavenge free radicals – charged particles that can damage cells, tissues and genetic material – which can affect your immunity.
Maintaining good blood levels of Vitamin C improves the function of the white blood cells that fight infections and may shorten the severity and duration of the common cold. Research at the University of Otago suggests 200mg daily as a minimum intake. It is found in high amounts in some fruits and vegetables but can be destroyed by cooking. Eating 2 kiwifruit, 2 oranges or a whole (raw) capsicum daily is a great way to get it.
Smokers, those who exercise intensively, and people subject to very stressful conditions may need more.
Interesting evidence begins to emerge supporting the use of vitamin C in people who are critically ill. Perhaps over the coming months we will see more support for this low-cost vitamin in treating viral illness.
Gut microbiome
Your intestinal tract is its own community with literally trillions of bacteria, fungi and other microorganisms. It also contains the largest pool of immune cells in the whole body.
Almost daily there is more information about the importance of the gut microbiome and how it communicates with, and may even regulate, immune cells. These cells, in turn have an important role in controlling how your whole immune system functions and how it responds to infection.
So, its’ not surprising that keeping these bacteria healthy may also keep your immune system functioning normally. Prebiotics and probiotics are the key players here.
While probiotics are the beneficial bacteria themselves, which are found in yoghurts, cultured cheeses and many fermented goods including kimchi, sauerkraut, kefir, miso and kombucha, prebiotics are essentially the non-digestible fibre that the bacteria feed on.
Prebiotics are found in a wide range of foods. Great sources are ground flaxseed, oat bran, apple pectin and complex carbohydrates such as those found in onions, beetroot, asparagus and artichokes. Polyphenols are also important for supporting a healthy microbiome – these are also found in a range of foods. Some are: green tea, olive leaves (make a tea from them), beetroot, blueberries, pomegranate and good quality extra virgin olive oil.
Omega 3
Omega 3s are required to form the membranes that surround each cell in your body and are associated with boosted B-cell activity which is a vital part of our immune system.
There are three forms of omega 3 fatty acids. One (called ALA) is “essential” meaning you need to consume it, as your body cannot make it. ALA is primarily found in plant oils, nuts and seeds. Flaxseed oil, or ground seeds of flax or chia are good sources. ALA is used to make other omega-3s, including EPA and DHA, which you can also get in their pre-formed state from oily fish.
B vitamins
Several members of the group of B vitamins are required for a normal immune response and a deficiency in them can alter the response of the immune system. Essentially, if you’re deficient in them, the body is less able to make antibodies, white blood cells and other immune factors that are used to fight infection. The most important ones are: pyridoxine (vitamin B6), cobalamin (vitamin B12) and folate (vitamin B9).
Vitamin B12 is needed to make red blood cells and cells of the immune system. It is naturally found in animal products, especially meat. Vegetarians and vegans are at high risk of a deficiency, as are those with digestive problems.
To absorb vitamin B12, you need vitamin B6, which can be found in foods including beef liver, chickpeas, fish such as tuna and salmon, cereals and onions. Small amounts also occur in rice, but the digestibility (and therefore availability) of it in rice is low.
Folate, which works as a cofactor in making blood cells, is required in balance with vitamin B12 for normal immune function, and low folate status has been implicated in poorer immune responses in the elderly. This vitamin is naturally present in a wide variety of foods, including dark green leafy vegetables, fruits, nuts, beans, seafood, eggs and meat. However, folate is destroyed by cooking, so you need to ensure you get some of these foods raw (or lightly steamed) wherever possible.

Exercise
Regular exercise has been found to enhance the body’s immune response and improve its defence activity. Regular, habitual exercise resets the immune system, something known as “immunoregulation”.
While the extent of this will clearly depend on the amount and type of exercise you do, we recommend a minimum of 150 minutes of moderate-intensity activity a week (that’s 30 minutes, 5 days a week) or 75 minutes of vigorous-intensity activity every week into your routine. If neither of these are possible, then aiming to walk at least 10,000 steps every day is advised.

Stress
While short-term stress may be beneficial for the immune system, chronic stress has been associated with the suppression of immunity.
The “fight or flight” type of acute stress causes a beneficial response in the immune system. This happens due to injuries that results in cuts, scrapes and bites – all potential sources of infection – so the immune system can protect from potential biological invaders.
However, consistently elevated cortisol, such as occurs with ongoing stress, is associated with suppression of the immune system. In animals, such immunosuppression increases vulnerability to disease and in humans chronic stress reduces the immune system’s capacity to produce antibodies following routine influenza vaccinations.
Moderate your alcohol intake
Alcohol can have a damaging effect on many aspects of human function and organs. Chronic alcohol use can increase the risks for heart disease as well as several cancers and can ultimately lead to liver disease.
Overconsumption of alcohol can also result in weakening of the immune system, reducing the number and function of cells that are important for the immune system–meaning you become more vulnerable to infections. Alcohol also has adverse effects on the gut; it upsets the normal balance of gut bacteria and disrupts the gut lining, making it easier for micro-organisms to get into the blood stream and from there to the liver. It also affects the way healthy gut microbes interact with the immune system. If you are drinking more than the recommended maximum of 2 units daily, we suggest reducing this. Substituting with kombucha or herbal teas is one way to help cut back.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3202617/
- https://www.frontiersin.org/articles/10.3389/fimmu.2020.01712/full https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7356429/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5707683/ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7356429/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6271412/ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4103721/\
- https://www.sciencedirect.com/science/article/pii/B9780323358682000177
- https://pubmed.ncbi.nlm.nih.gov/11697022/
CATEGORIES
SEARCH
LATEST POSTS



Too much of a good thing?

Periods Matter

Light – A New Ally for Healing
Related Posts
GIVE YOUR BRAIN SUPER MEMORY Anyone can improve their memory using a proven scientific method the ancient Greeks and Romans developed. The



