Could You Have a Histamine Intolerance?
- By Sharon Erdrich
- Digestive Health, Immune Function, Nutrition, Topics
Histamine intolerance is surprisingly common.
There are two main levels of intolerance: the first is associated with food and often results in digestive problems. The second is more systemic and can cause a wide range of symptoms, including hives, flushing, low pain tolerance, sweating, excess mucous production and seasonal allergies. It may result cause hyperactivity, compulsiveness and depression. The variable and wide range of symptoms is because the receptors for histamine are found in multiple sites in the body. The symptoms of histamine intolerance can manifest in:
- the digestive system, with diarrhoea, abdominal pain, cramps, bloating, reflux
- the respiratory tract with sneezing, mucous, congestion, cough, asthma
- the heart, with irregular or fast heartbeat (sometimes called palpitations),
- the nervous system – causing headache, dizziness, anxiety, sleep disturbances
- reproductive tissues or organs. This can be underlying painful periods, menstrual headaches and so on,
- as well as the skin with redness, itching, flushing.
Most people know histamine as the thing to counteract when a person has an allergic reaction such as hay fever, etc taking some form of antihistamine. Histamine is released by cells in the body in response to damage or a perceived threat. Once released it causes swelling, redness and heat and acts as a signal for other immune system factors to come to the scene to help. But histamine also has other roles in the body, including regulating stomach acid and stimulating the brain. As well as all this there is an interaction between female hormones and histamine.

Histamine in Food
Almost all food has the potential to contain, or stimulate the release of histamine. Histamine is produced in food as the result of ageing and bacterial degradation. Some food reactions that suggest histamine intolerance include aged cheese, fish or seafood, deli meats, eggs (especially the whites), fermented foods (such as sauerkraut) and avocado. The older the food (or more aged) the higher the potential histamine content. Some food has the potential to aggravate the gut and cause a histamine release. Citrus fruits are commonly implicated in this, as are mineral supplements containing citrates. For people with histamine intolerance, alcohol commonly aggravates the problems, resulting in facial flushing, a blocked nose and may also cause headaches. So if “wine & cheese” sets you off, this is a good clue to having a histamine intolerance.

What’s Behind Histamine Intolerance?
Contrary to what you might think (or have been told), the food is not actually the problem. The body has methods to break down histamine – after all, we didn’t evolve with refrigerators and preservatives!
The first histamine-degrading subtance is an enzyme that is produced in the lining of the intestines, called diamine oxidase (DAO). It’s primary job is to break down histamine in our food. If the gut wall is damaged in any way, or if there are certain nutrient deficiencies, this enzyme may not be produced in adequate amounts and the histamine may aggravate the gut, causing symptoms similar to irritable bowel syndrome, and is also absorbed into the blood stream. Once in the blood stream, histamine is normally broken down by another enzymatic process involving N-methyltransferase (HNMT) and eliminated from the body.
Another common factor is under-methylation. Methylation is a complex biochemical reaction that is on-going in the body and involved in the metabolism of vitamins, hormones, neurotransmitters and more. Removing histamine required methyl groups, and when histamine is high, these groups get depleted, which further exacerbates the problem.
Histamine intolerance occurs when there is either too much histamine being ingested or liberated, or not enough being broken down—or both! Any inadequacy in the clearance mechanisms – either in the gut or in the blood stream – can cause the symptoms of histamine intolerance.
How does Histamine Interact with Hormones?
Women may notice that their tolerance (or intolerance) changes throughout their menstrual cycle, or disappear when pregnant. This is because of a number of different hormonal interactions.
- Progesterone, which is high in the second half of the menstrual cycle and very high during pregnancy), up-regulates DAO. This means more DAO, and more histamine breakdown early in the luteal phase (soon after ovulation) when progesterone is high.
- Oestrogen down-regulates DAO. So an excess, or relative excess of oestrogen is associated with increased histamine intolerance.
- Some forms of hormonal birth control (those containing oestrogen) cause an oestrogen excess and progesterone deficiency – one reason some women do better on a progesterone-only contraceptive.
Normally, your body regulates histamine by making it, and then by clearing it. . . It’s a fine balance between “histamine in” and “histamine out”. Histamine also boosts libido, which helps explain oestrogen’s effect on increasing sex drive, while antihistamines decrease it.
During pregnancy, not only is progesterone very high, but the placenta makes large amounts of DAO. Women often report that histamine intolerance, allergies and food sensitivities improve during pregnancy.
Reasons for Poor Histamine Clearance
There are several reasons for a diminished ability to clear histamine. These include:
- Genetic variant of the histamine-clearing enzymes HNMT and DAO.
- Genetic variant of key enzymes involved in methylation, resulting in poor HNMT function. This can be tested using a comprehensive health genetics test, such as OPUS23
- SIBO (small intestinal bacterial overgrowth) because it can damage the lining of the intestine and impair production of diamine oxidase
- Vitamin B6 deficiency: an essential cofactor for the formation of DAO.
- Copper deficiency: Copper is an essential co-factor for the formation of DAO
- An excess of oestrogen, which down-regulates DAO.
- Progesterone deficiency (progesterone up-regulates DAO).
- Hormonal birth control (oestrogen excess and progesterone deficiency).
What can be done about Histamine Intolerance?
Firstly, a consultation with a health consultant can help you determine the underlying cause. While avoiding high histamine foods is a fast way to feel better, it is a very restrictive diet and difficult to maintain in the long term. Long term dietary restrictions are not advised, as this can lead to nutrient deficiencies. By addressing underlying issues, most people find that they are able to consume histamine foods.

Hypersensitive or overly reactive skin can indicate problems associated with histamine.
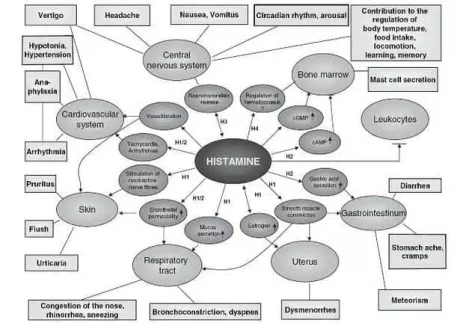
Histamine has many roles in the body. An excess of it can manifest in a variety of ways.
Identify and Address the Cause, or Causes
Depending on the individual cause the treatment strategy can vary. For women with appreciable fluctuations in histamine intolerance associated with the menstrual cycle, an important strategy is to promote the healthy detoxification of oestrogen. Find out if you have genetic variants that mean that oestrogen clearance is compromised (COMT, CYP1A1, CYP1B1). We recommend natural treatments to support healthy progesterone levels. This can include herbal medicine and vitamin supplementation. We can also use salivary hormone mapping (over the course of the menstrual cycle) to determine the role of the levels of progesterone and oestrogen.
Ensuring adequate intake of vitamin B6 is important because this vitamin supports healthy progesterone metabolism and upregulates DAO. Food sources of vitamin B6 include meat, chicken, and sunflower seeds.Most people will have some kind of gut involvement – so identifying and correcting dysbiosis and/or small intestinal bacterial overgrowth (SIBO) is important. Avoiding food that may aggravate a histamine release such as gluten and A1 casein (dairy) is also helpful to support the healing phase. These common foods trigger histamine release. Most New Zealand milk is A1, but A2 milk is available at some supermarkets.
Make an appointment now to discuss the factors contributing to your histamine intolerance and let food start being your friend again!
Choose your practitioner, then the appointment type to see the available times.
CATEGORIES
SEARCH
LATEST POSTS



Too much of a good thing?

Periods Matter

Light – A New Ally for Healing
Related Posts
What is Fibromyalgia? Simply put, fibromyalgia (also referred to as fibro) is a syndrome with a constellation of symptoms, central of which
What does it take to have strong and healthy bones? Ultimately – excellent lifestyle and nutrition. In an ideal world we would
GENERAL REQUIREMENTS FOR BREATH TESTING What’s on this page: General instructions General preparation Medications/Supplements Dietary preparation The diet Meal ideas Gluten-free bread