Faecal Microbial Transplant (FMT), which is also known as stool transplant or bacteriotherapy, is a procedure in which faecal matter, or stool, is collected from a healthy person and administered into the intestines of another person. Interestingly, transfering donor faeces by way of “yellow soup” to a recipient with gut diseases dates back to the 4th century in China!
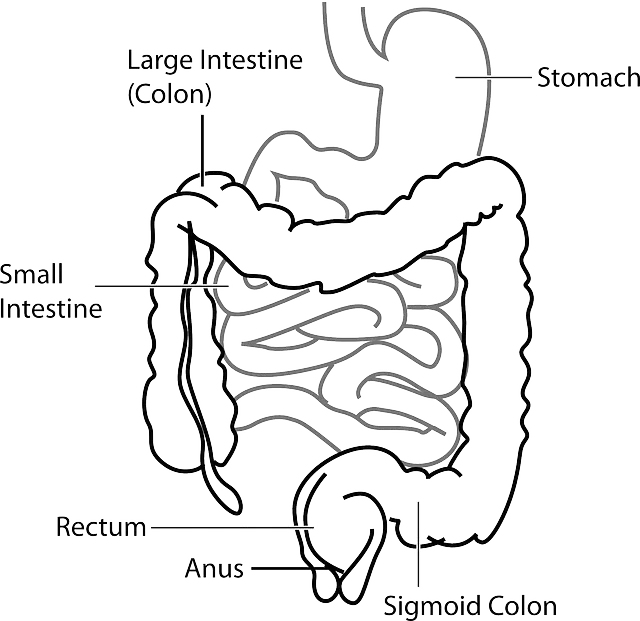
In FMT, the donor stool is given either by mouth (though a tube into the intestine, or in “Crapsules”) or via the rectum (enema) or during colonoscopy.
Preliminary studies suggest that FMT may be an effective therapy in Crohn’s disease, but so far, this is not widely available as a treatment.