
Vitamin Sunshine
- By Sharon Erdrich
- Bones, Joints & Muscles, General Health, Immune Function, Mental Health, Nutrition
In an ideal world, by summer’s end your stocks of Vitamin Sunshine (vitamin D) levels will have attained a high enough level to get you through the winter, but for an increasing number of New Zealanders that may not be the case.
Vitamin D is a trace substance and must be produced or ingested in a certain quantity to ensure good health. As with other nutrients, deficiency results in specific diseases, in this case rickets (in young children), and osteomalacia (softening of the bones) in older children and young adults. The softened bones of children and young adults with osteomalacia can lead to the bones bending during growth, becoming bowed. This is more apparent in the bones that carry weight, especially in the legs. Osteomalacia in older adults can lead to fractures. But vitamin D is unique in that it is actually a hormone and we are designed to make it ourselves – with help from the sun!
Ultraviolet B light waves (UVBs) activate cholesterol in the skin to make the vitamin form. This is then changed in the liver before being converted into its active form in the kidneys and several other tissues, including the breasts, prostate gland and in the bowel.
Approximately a hundred years ago, vitamin D was recognised as being important for bone health, and the major focus of vitamin D-related research has, until more recent years, been in the area of calcium metabolism and bones. Read our blog “15 Myths about Vitamin D”
Down to the bone
The most dramatic effect of vitamin D is the enhancement of the absorption of calcium in the intestines (as well as stimulating absorption of both phosphate and magnesium) which is then used in bone metabolism.
Severe vitamin D deficiency due to inadequate sun exposure in the 19th century produced an epidemic of rickets, resulting in growth retardation, muscle weakness, skeletal deformities, low blood calcium levels, tetany (cramps and/or muscle spasms) and seizures. The encouragement of sensible sun exposure and the fortification of milk with vitamin D resulted in an almost complete eradication of the disease.
However, vitamin D deficiency has again become an epidemic in children, and rickets has become a global health issue. In addition to causing rickets, low vitamin D prevents children from attaining their genetically programmed peak bone mass, contributes to and exacerbates osteoporosis in adults, and causes the often painful bone disease, osteomalacia.

Beyond rickets
There is a growing mountain of evidence that, even before birth as well as during a person’s lifetime, vitamin D plays a role in the prevention of several chronic diseases of which multiple sclerosis and schizophrenia are the most studied. Both conditions have higher rates of occurrence in countries closer to the poles and in dark-skinned people living at higher latitudes.
Receptors for the vitamin have been found in a wide variety of tissues in the body and a variety of conditions, including depression, seasonal affective disorder (SAD, or the ‘Winter Blues’), Parkinson’s disease, various autoimmune disorders, gingivitis (gum disease), insulin resistance, cardiovascular disease, diabetes, high blood pressure, heart failure, infl uenza, psoriasis, gout, interstitial cystitis, decreased pulmonary function, chronic kidney disease, pancreatitis, rheumatism, hepatitis B, haemochromatosis, gastrointestinal diseases and many common cancers, particularly of the breast, colon and prostate, have been connected to inadequate vitamin D. Conversely, an adequate supply of vitamin D seems to reduce the incidence rates or improve the prognosis of several cancer forms, including prostate, breast and colon cancer, as well as of lymphomas.
Vitamin D has a direct action on muscle function and is vital for muscle contraction, thus a deficiency can cause impaired muscle function and muscle weakness which may lead to falls in the elderly, general clumsiness, and a drop in athletic performance – especially during winter. These conditions are reversible following vitamin D supplementation.
The Importance of Vitamin D in Immunity
The most common infections affecting most people are the common cold and influenza, which are caused by viruses. Being deficient in vitamin D increases the risk for respiratory infection. Low blood concentrations of vitamin D is associated with increased susceptibility to acute respiratory tract infections (generally viruses), and vitamin D supplementation can reduce the risk of such infections in both children and adults.


When can a deficiency occur?
- When usual intake is below recommended levels.
- When there is limited exposure to sunlight.
- When the kidney cannot convert vitamin D to it’s active hormone form.
- When someone cannot adequately absorb vitamin D from the digestive tract, such as happens with Coeliac disease, small intestinal problems (e.g., short bowel syndrome, bowel surgery)
Am I at risk?
Season, time of day, exposure time, latitude, altitude, the amount of skin surface exposed, ageing, body fat, sunscreen use, certain skin conditions and skin pigmentation all influence the production of vitamin D. Clouds, pollution, smog, glass and ozone can block UVB.
What about skin cancer?
We know that excess sun exposure increases your chance of getting sunburnt, which is a strong risk factor for skin cancer. This is a big issue in New Zealand and Australia. However, research has shown that vitamin D deficiency increases the risk of cancer, including skin cancer. Furthermore, if you are diagnosed with melanoma, the tumours are likely to be deeper (more advanced) if you are vitamin D deficient.
Our recommendation is safe, sensible sun exposure. A rule of thumb is letting the rays of the sun warm up your arms and legs, or arms and upper torso daily for half of the amount of time it would take for you to go pink. This way you don’t damage your skin and can modify your time in the sunshine to meet your skin-type.
Read our blog “15 Myths about Vitamin D”

Can I test my level of Vitamin D?
To determine adequate vitamin D, a blood test (currently self-funded in New Zealand for most people) is required. We recommend testing twice a year until you get the right balance of sun and/or supplements. It is important to realise, that in spite of an abundance of evidence supporting higher vitamin D concentrations, the “normal” parameters in New Zealand remain at levels set many years ago and have not been revised for a very long time. The optimal range is 75-125nmol/L.
Undertaking a more comprehensive group of blood tests that measure calcium, phosphorus, alkaline phosphatase and parathyroid hormone can help form a more complete picture.
For those with risk of not converting vitamin D into the active form (determined by your genetics), both forms can be tested. Contact us to find out how.
People most at risk of developing a deficiency include:
- Dark-skinned people living in a temperate climate.
- Those who, for cultural reasons, keep their skin covered.
- Those using sunscreen-containing skin care products all year round.
- Those using SPF products with ratings greater than eight as it effectively blocks synthesis of vitamin D.
- People with an inherited vitamin D disorder, causing genetic rickets.
- Shift workers (especially those who sleep during the day).
- The elderly, infirm or those in care facilities.
- Those with skin conditions, including having suffered severe burns.
- Pregnant women.
- Infants and children (especially if born to a vitamin D-deficient mother).
- Infants fed only breast milk for an extended period – higher risk if mum is vitamin D deficient
- Epileptics on certain medications.
- Those with compromised kidney function.
- Those with a milk allergy or lactose intolerance.
- The obese (vitamin D is stored in fat tissue, so it’s not readily available)
- Those with metabolic syndrome and insulin resistance.
- Those who have had surgery to remove all or part of their stomach or gall bladder.
Other factors that impair the uptake of dietary vitamin D:
- Strict vegetarianism and veganism.
- Avoidance of dairy products and/or fish.
- Intestinal malabsorption.
But remember, diet is not the best way to get your vitamin D.


Image Credit: Vegan Liftz
How common is the problem?
- There are several issues when identifying people with vitamin deficiency:
- The test is expensive compared to the cost of supplementation and it not funded by our health care system for most people.
- Doctors are discouraged from performing it and many doctors do not consider testing for it unless a patient has osteomalacia or osteoporosis.
- Currently, lab reports state the target range for blood levels of vitamin D is 50-150nmol/L, yet recent research suggests 75-125nmol/L is the ideal range for optimal functioning of the vitamin.
Inadequacy has been reported in approximately 36 per cent of otherwise healthy young adults and up to 57 per cent of general medicine patients (in the United States). Eighty-seven per cent of pregnant women in New Zealand had levels below 50 (61 per cent were below 25!); these figures are not confined to veiled women or women with dark skin. In a New Zealand outpatients clinic, 78 per cent of patients were below the reference range and 22 per cent of these had moderate to severe deficiency (less than 25), approximately 50 per cent of school children (age five to 14 years) were below the lower limit threshold. Bearing in mind that those statistics relating to deficiency are based on a cut-off point of 50, so true deficiency figures could be a lot higher.
Dietary sources of Vitamin D
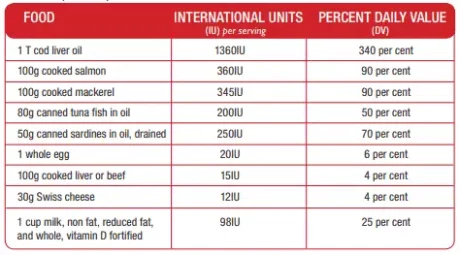

Note, all of the above are from animal sources. However, some vitamin D-enriched foods such as rice milk are also available. The DV for vitamin D in this chart is 400IU for adults which is by current research, very low. If you totally avoid the sun, you may need about 4000 units of vitamin D a day! Which means you can’t get enough vitamin D from milk (unless you drink 40 glasses a day) or from a multi-vitamin (unless you take about 10 tablets a day), neither of which is recommended. Our practitioners are experts in figuring out your individual needs.
Finally..
Most of us produce about 20,000 units of vitamin D after about 20 minutes of summer sun. This is about 100 times more vitamin D than the daily Recommended Dietary Intake (RDI). If you don’t get vitamin D from sunshine the way Mother Nature intended, you need to take supplemental vitamin D3. Just how much depends on what your levels currently are, but you can be sure that they’re low if you’ve been avoiding the sun.
For more information and research go to www.vitamindcouncil.com
Note: this is an updated version of a similar article written by Sharon Erdrich, published in Healthy Options magazine, 2007


References
- https://pubmed.ncbi.nlm.nih.gov/30901909/
- https://pubmed.ncbi.nlm.nih.gov/31101452/
- https://pubmed.ncbi.nlm.nih.gov/29480918/
- https://pubmed.ncbi.nlm.nih.gov/26822497/
- https://pubmed.ncbi.nlm.nih.gov/26521023/
- https://pubmed.ncbi.nlm.nih.gov/28216084/
- https://onlinelibrary.wiley.com/doi/full/10.1111/apt.15777
- https://www.mdpi.com/2072-6643/12/4/1181
CATEGORIES
SEARCH
LATEST POSTS



Too much of a good thing?

Periods Matter




