Allergies & Food Intolerances
- By Sharon Erdrich
- Digestive Health, Immune Function, Nutrition
Allergies and food intolerances disrupt your life and can make you miserable.
The long-term consequences of undiagnosed and untreated allergies include just about anything due to the constantly elevated level of inflammation and the generation of free radicals that damage tissues and organs. In addition, people with allergies are more likely to develop more allergies, increasing the misery and the long-term health risks.
What is an allergy?
Allergies occur when the body’s immune system (which has the important role of protecting us from foreign invaders) reacts to non-threatening substances such as food or pollen, as if they were harmful. This can cause chemical reactions in the body which sufferers experience as unpleasant (and sometimes life-threatening) symptoms.
It’s important to be aware that reactions to food-related reactions are not necessarily allergies. The can also be classed as intolerances.
Adverse reactions to food can be divided into five distinct groups.
- Classic, true food allergy, such as peanut anaphylaxis – where there is an immediate IgE-mediated reaction. This will require emergency adrenaline injections and may necessitate medical resuscitation.
- Delayed food allergies are sometime referred to as “hidden”, or “masked” allergies. The reaction to the causative foods can take up to several days to manifest and may take much longer to resolve following removal of that food from the diet.
- Food intolerances. Generally these are not immune mediated but may be due to enzyme deficiencies, and other mechanisms that mimic true allergic reactions. There is some evidence that one type of food intolerance may be due to activation of the immune system. This is controversial.
- Contaminants or poison present in food can cause toxic reactions in some people. These reactions are usually recognisable.
- Food aversion occurs when a person is convinced that they are allergic to a food, but when challenged with the food, fail to have any reaction.
True Food Allergies
True Food Allergy, is an immediate IgE-mediated reaction, and can constitute a medical emergency when activated. A small protein particle (called an allergen) is responsible for triggering the antibody response – this causes mast cells to release histamine, resulting in tissue inflammation and swelling.
An antibody called Immunoglobulin E (IgE) accounts for 90% of true food allergic reactions. A reaction can occur even to tiny traces of the offending allergen in exquisitely sensitive individual. Even airborne food allergens can trigger anaphylaxis – this is most commonly known in relationship to peanut allergy.
Classical IgE-mediated food allergy can present with immediate red skin rashes, swelling of the face and neck and even anaphylaxis with shock and circulatory collapse. In adults, the foods most commonly implicated in anaphylaxis are wheat, soy, milk, peanuts, tree nuts, shellfish, fish and egg (white).
Exacerbations of eczema and rhinitis can occur in food allergy. Vomiting and diarrhoea, oesophagitis can also occur. Frequently patients think they are allergic to one food but may actually be allergic to three or more foods.
Oral Allergy Syndrome occurs when allergic reaction is localised to the mouth and throat and is triggered by fruit and vegetables such as apple, peach, celery, tomato and cherry.

Delayed Allergies
Delayed T-cell mediated food allergic reactions are typically seen with contact dermatitis and Coeliac Disease and can take 24 hours or more to evolve. These types of reactions do not involve IgE antibodies. IgG-mediated reactions are very common and usually undiagnosed.
Research has confirmed a connection between IgG or delayed allergy and inflammatory bowel conditions such as Irritable Bowel Syndrome. IgG antibodies can be measured to identify the specific foods implicated.
Food Intolerance (Non-allergic food hypersensitivity)
Food intolerance is an adverse reaction that does not involve the immune system. Reactions are dose-dependant, meaning that smaller amounts of the offending food may be tolerated, but at a certain dietary threshold a reaction occurs.
There are a number of different reasons food intolerance can occur. For example, a deficiency in a digestive enzyme such as lactase results in lactose (milk sugar) intolerance. When lactase (the enzyme that enables us to digest lactose) is depleted the result can be cramping, flatulence and frothy diarrhoea after drinking cows milk, or more moderate symptoms from smaller doses of lactose (such as from milk or milk powder added to many bread products).
Lactose intolerance can affect up to 20% of the population, often begins in teenage years and tends to get worse with advancing age. Lactose intolerance is more common in Asians, African, Hispanic and people from the Mediterranean region. This kind of food intolerance is best managed by avoiding the food or taking a dietary supplement that contains the missing enzyme.
Intolerance to sucrose in table sugar and fruit can lead to similar symptoms if there is a deficiency of the intestinal enzyme which breaks sucrose down to absorbable fructose and glucose.
Fructose is one of the natural sugars in fruit and corn. Fructose consumption commonly causes gas, bloating, diarrhoea and other gastro symptoms. The ratio of fructose to glucose is a key factor in how well these fruits are tolerated. Common aggravators are stonefruit (peaches, nectarines etc.), watermelons and mango. You can order tests for sugar (lactose, fructose, sucrose) intolerances here
For some people, the types of foods causing reactions seems vast. Common examples include apples, onions, beans (such as kidney beans), whole grains, some nuts and so on. For many people the problem lies in the digestive system itself, rather than the food. Read more here.

Histamine Intolerance
Even good food can cause unwelcome reactions!
Some foods naturally contain high levels of a potentially problematic molecules, called amines. The most common of these is histamine. Most people are familiar with histamine from the view point of hayfever, insect bite reactions etc. But food can be a source of histamine as well. Examples of foods high in histamine include eggs, nuts, olives, alcohol, seafood, aged cheeses, some vinegars, processed/aged meat and fermented foods. Reactions are varied – from digestive disturbance to sinus or throat symptoms, skin rashes (commonly red and itchy) and headaches. Read more about histamine intolerance here.
Food Toxic Reactions & Food Additives
Food Toxic reactions have no immune basis, but are due to bacterial endotoxins and contaminants. This results in vomiting, diarrhoea, flushing and certain neurological symptoms in all individuals who consume the food.
Other biologically active toxins include algae that infest shellfish with paralytic neurotoxins, glyco-alkaloids in potatoes and amatoxin in mushrooms. Mycotoxins in grain produce such as wheat, rye, barley and oats can cause Ergotism with gangrene and convulsions. Scromboid toxicity occurs when fish putrefies and releases histamine causing allergy-like reactions.
Food additives such as colourants and preservatives may trigger pseudo-allergic reactions. These are not IgE mediated, but possibly involve direct release of histamine from specialised cells in the body. Histamine occurs naturally in many foods and when absorbed in the GI tract, can trigger an allergic-like reaction. A similar reaction can also be seen with naturally occurring dietary salicylate in aspirin-sensitive people. Other chemicals found in food can cause ill effects such as caffeine induced palpitations. Capsaicin in chili induces a typical “hot curry” burning sensation in the mouth, and alcohol-induced flushing and nasal congestion is due to local vasodilatation. Many of these reactions are related to your genetics.
Allergy vs Intolerance
As detailed above, an allergy is mediated by the immune system, and markers for such reactions can be measured in the blood. Allergy diagnosis is best made by your doctor or allergy specialist. An intolerance is often completely confined to within the gastro-intestinal tract and thus is NOT detectable by a blood test. The gold standard for this kind of problem is elimination and provocation testing.
SYMPTOMS THAT MAY BE ASSOCIATED WITH FOOD-RELATED PROBLEMS
DIGESTIVE SYSTEM
- Indigestion
- Nausea
- Vomiting
- Irritable Bowel Syndrome
- Diarrhoea
- Constipation
- Gas
- Bloating
- Reflux
- Pruritus ani (itchy anus)
- Cramping pain
- Colic (in babies)
Urinary Tract
- Frequent urination
- Burning
- Bedwetting in children
Cognitive & Psychological
- Mood swings
- Anxiety
- Depression
- Food cravings
- Poor concentration
- Fatigue
- Hyperactivity
- Cranky behaviour in children
Head & Neck
- Ear infections
- Runny or congested nose
- Recurrent sinusitis
- Headaches
- Migraines
- Sore throat
- Mouth sores
Chest
- Asthma
- Irregular heart beat
Muscle and Joints
- Muscle aches
- Joint pain
- Joint inflammation (arthritis)
- Some cases of rheumatoid arthritis
- Water retention
- Weight gain
- Eczema
- Hives
- Rashes
- Excess perspiration
Identifying Allergies
There seems to be so many people offering all kinds of tests available to detect food allergies that it can be very difficult to know where to start. Your doctor or allergy specialist will use some tests to assess immediate (IgE) allergies, however this can inconclusive due to the wide variety of possible reactions.
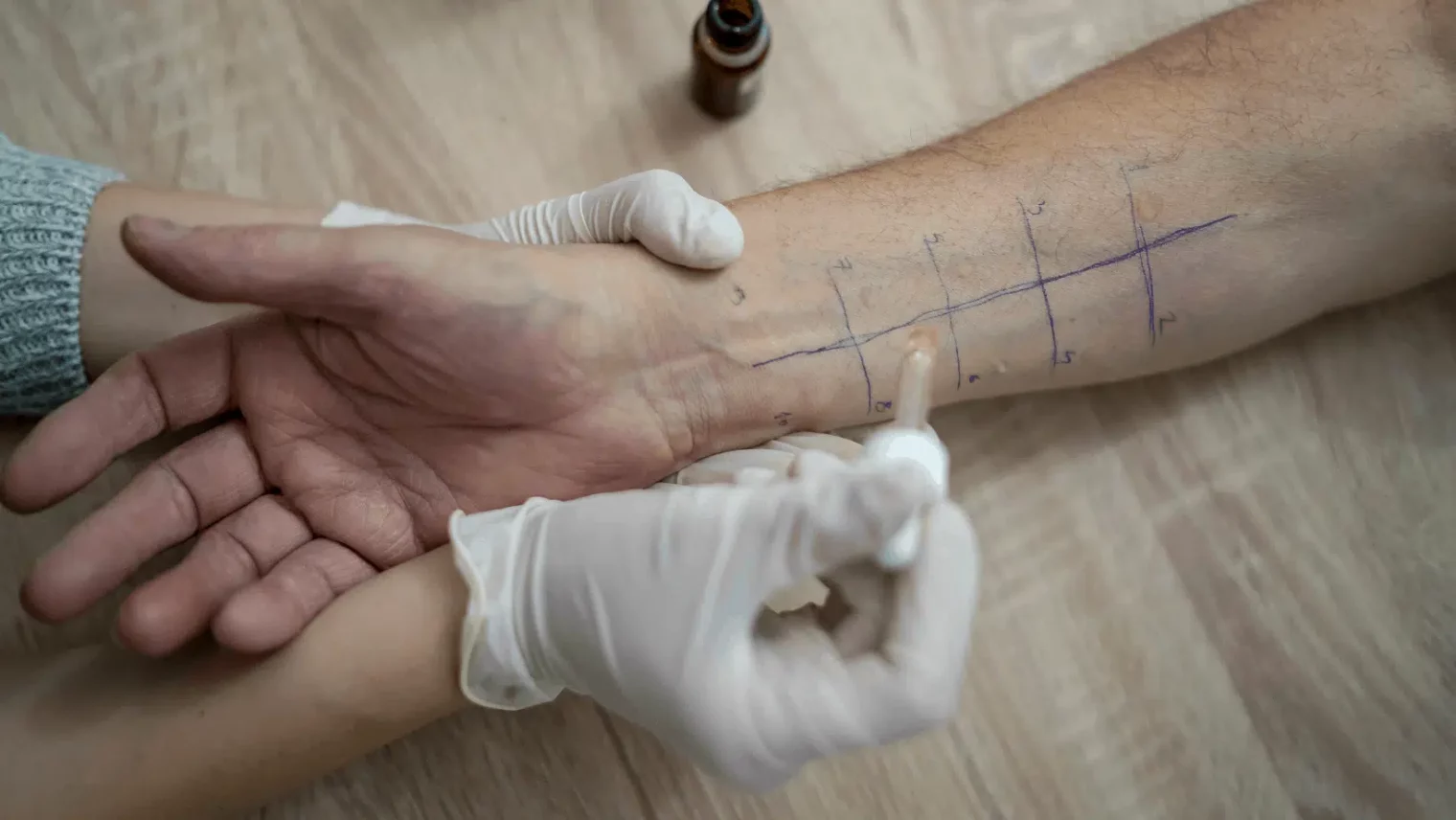
The SKIN PRICK Test
This test is available at the lab (you can request via your doctor or we can arrange this for you). The test involves using a small needle to prick the skin and introduce a drop of fluid containing a known allergen. The reaction – noted within the next half hour will help identify reactions that provoke a histamine release to a limited number of allergens. The usual substances tested include dust mites, animal hair, various pollens and highly suspect foods. However, not all food allergies will show up here as a) the antibodies are not so concentrated in the skin and b) not all allergic reactions are immediate.
A Standard BLOOD TEST
A single measure of IgE in the blood is a fair indicator of an IgE-mediated response, but does not pinpoint the culprit.
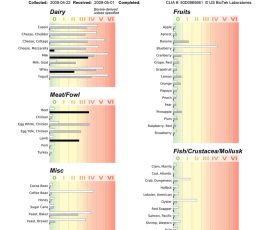
If IgE is elevated, to verify specific reactions a subsequent sample of blood is taken and sent to the laboratory for what is known as the ‘RAST’ (Radio AllergoSorbent Test). This measures the amount of specific IgE antibodies (which trigger a histamine release) in your blood to various environmental and food allergens. House dust mite IgE will be raised if you have an allergy to house dust mites and the result is then graded, depending on the level of that particular IgE in the blood.
Over 400 different allergens can be tested for in this way, but usually only half a dozen or so of the most likely culprits are tested due to the cost – between $24 and $30 for each item tested.
The ELIMINATION AND CHALLENGE TEST: Considered by allergists to be the “gold standard” – the diet is reduced down to a minimal “low-reactive” diet until symptoms have abated. Then foods are gradually reintroduced in a controlled manner and symptoms are noted. This method is very effective but is also very difficult to comply with and can weeks or months to test all foods.
At House of Health we can guide you through the Elimination & Challenge test, providing comprehensive support as you go through the process. We also offer a comprehensive medical blood test that is sent to a laboratory in the United States for IgE and IgG antibodies to at least 96 different foods. Options are outlined here. However, in our experience, the test results can mislead you into believing that the food is the problem, when in reality it tends to be the digestive system(except for immediate onset, IgE reactions) that is the issue.
Controversial Tests
Some practitioners perform tests that have no acceptable degree of reliability on repeated testing. They shouldn’t be relied on for allergy diagnostic purposes as they are of an inferior nature according to the British Society for Allergy and Clinical Immunology.
VEGA testing involves the measurement of disordered electromagnetic currents in the body to certain substances. Results are very unreliable according to the British Medical Journal.
APPLIED KINESIOLOGY tests muscle strength in the presence of various allergens, with a loss of strength indicating an allergy. This test is equally unreliable according to the British Society for Allergy and Clinical Immunology. However, in some cases, with a very experienced practitioner, we believe that this method may be of value.
HAIR ANALYSIS involves testing a hair sample in either a VEGA or EAV machine, testing for energy fluctuations according to various substances. These methods have been assessed and found to be unreliable to diagnose allergy.

What Can You Do?
So, you think (or know) you have a food intolerance – it’s time to contact us. We will take a full clinical history from you including your symptoms, details of when they occur and any other relevant information. Some food-related problems can be pinpointed without any further testing. We will then be able to offer you advice requiring diagnostic testing and support options to help minimise your symptoms, plus dietary and other practical advice.
Featured Product
CATEGORIES
SEARCH
LATEST POSTS



Too much of a good thing?

Periods Matter

Light – A New Ally for Healing
Related Posts
Irritable Bowel Syndrome (IBS) is a common digestive problem characterised by symptoms like abdominal pain, bloating, and altered bowel habits. However, there